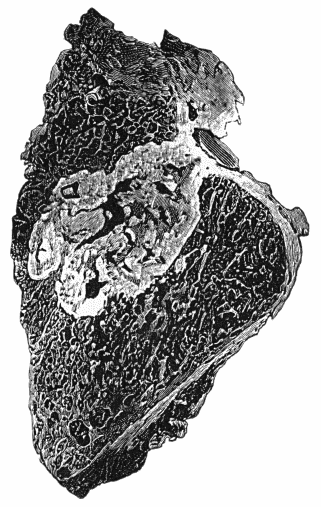
Fig. 156.—Section of Upper End of Fibula, showing caseating focus in marrow, erupting on articular surface and infecting joint.
Tuberculous disease of joints results from bacillary infection through the arteries. The disease may commence in the synovial membrane or in the marrow of one of the adjacent bones, and the relative frequency of these two seats of infection has been the subject of considerable difference of opinion. The traditional view of König is that in the knee and most of the larger joints the disease arises in the bone and in the synovial membrane in about equal proportion, and that in the hip the number of cases beginning in the bones is about five times greater than that originating in the membrane. This estimate, so far as the actual frequency of bone lesions is concerned, has been generally accepted, but recent observers, notably John Fraser, do not accept the presence of bone lesions as necessarily proving that the disease commenced in the bones; he maintains, and we think with good grounds, that in many cases the disease having commenced in the synovial membrane, slowly spreads to the bone by way of the blood vessels and lymphatics, and gives rise to lesions in the marrow.
Morbid Anatomy.—Tuberculous disease in the articular end of a long bone may give rise to reactive changes in the adjacent joint, characterised by effusion and by the extension of the synovial membrane over the articular surfaces. This may result in the formation of adhesions which obliterate the cavity of the joint or divide it into compartments. These lesions are comparatively common, and are not necessarily due to actual tuberculous infection of the joint.
The infection of the joint by tubercle originating in the adjacent bone may take place at the periphery, the osseous focus reaching the surface of the bone at the site of reflection of the synovial membrane, and the infection which begins at this point then spreads to the rest of the membrane. Or it may take place in the central area, by the projection of tuberculous granulation tissue into the joint following upon erosion of the cartilage (Fig. 156).

Fig. 156.—Section of Upper End of Fibula, showing caseating focus in marrow, erupting on articular surface and infecting joint.
Changes in the Synovial Membrane.—In the majority of cases there is a diffuse thickening of the synovial membrane, due to the formation of granulation tissue, or of young connective tissue, in its substance. This new tissue is arranged in two layers—the outer composed of fully formed connective or fibrous tissue, the inner of embryonic tissue, usually permeated with miliary tubercles. On opening the joint, these tubercles may be seen on the surface of the membrane, or the surface may be covered with a layer of fibrinous or caseating tissue. Where there is greater resistance on the part of the tissues, there is active formation of young connective tissue which circumscribes or encapsulates the tubercles, so that they remain embedded in the substance of the membrane, and are only seen on cutting into it.
The thickened synovial membrane is projected into the cavity of the joint, filling up its pouches and recesses, and spreading over the surface of the articular cartilage “like ivy growing on a wall.” Wherever the synovial tissue covers the cartilage it becomes adherent to and fused with it. The morbid process may be arrested at this stage, and fibrous adhesions form between the opposing articular surfaces, or it may progress, in which case further changes occur, resulting in destruction of the articular cartilage and exposure of the subjacent bone.
In rare instances the synovial membrane presents nodular masses or lumps, resembling the tuberculous tumours met with in the brain; they project into the cavity of the joint, are often pedunculated, and may give rise to the symptoms of loose body. The fringes of synovial membrane may also undergo a remarkable development, like that observed in arthritis deformans, and described as arborescent lipoma. Both these types are almost exclusively met with in the knee.
The Contents of Tuberculous Joints.—In a large proportion of cases of synovial tuberculosis the joint is entirely filled up by the diffuse thickening of the synovial membrane. In a small number there is an abundant serous exudate, and with this there may be a considerable formation of fibrin, covering the surface of the membrane and floating in the fluid as flakes or masses; under the influence of movement it may assume the shape of melon-seed bodies. More rarely the joint contains pus, and the surface of the synovial membrane resembles the wall of a cold abscess.
Ulceration and Necrosis of Cartilage.—The synovial tissue covering the cartilage causes pitting and perforation of the cartilage and makes its way through it, and often spreads widely between it and the subjacent bone; the cartilage may be detached in portions of considerable size. It may be similarly ulcerated or detached as a result of disease in the bone.
Caries of Articular Surfaces.—Tuberculous infiltration of the marrow in the surface cancelli breaks up the spongy framework of the bone into minute irregular fragments, so that it disintegrates or crumbles away—caries. When there is an absence of caseation and suppuration, the condition is called caries sicca.
The pressure of the articular surfaces against one another favours the progress of ulceration of cartilage and of articular caries. These processes are usually more advanced in the areas most exposed to pressure—for example, in the hip-joint, on the superior aspect of the head of the femur, and on the posterior and upper segment of the acetabulum.
The occurrence of pathological dislocation is due to softening and stretching of the ligaments which normally retain the bones in position, and to some factor causing displacement, which may be the accumulation of fluid or of granulations in the joint, the involuntary contraction of muscles, or some movement or twist of the limb. The occurrence of dislocation is also favoured by destructive changes in the bones.
Peri-articular tubercle and abscess may result from the spread of disease from the bone or joint into the surrounding tissues, either directly or by way of the lymphatics. A peri-articular abscess may spread in several directions, sometimes invading tendon sheaths or bursæ, and finally reaching the skin surface by tortuous sinuses.
Reactive changes in the vicinity of tuberculous joints are of common occurrence, and play a considerable part in the production of what is clinically known as white swelling. New connective tissue forms in the peri-articular fat and between muscles and tendons. It may be tough and fibrous, or soft, vascular, and œdematous, and the peri-articular fat becomes swollen and gelatinous, constituting a layer of considerable thickness. The fat disappears and is replaced by a mucoid effusion between the fibrous bundles of connective tissue. This is what was formerly known as gelatinous degeneration of the synovial membrane. In the case of the wrist the newly formed connective tissue may fix the tendons in their sheaths, interfering with the movements of the fingers. In relation to the bones also there may be reactive changes, resulting in the formation of spicules of new bone on the periosteal surfaces and at the attachment of the capsular and other ligaments; these are only met with where pyogenic infection has been superadded.
Terminations and Sequelæ.—A natural process of cure may occur at any stage, the tuberculous tissue being replaced by scar tissue. Recovery is apt to be attended with impairment of movement due to adhesions, ankylosis, or contracture of the peri-articular structures. Caseous foci in the interior of the bones may become encapsulated, and a cure be thus effected, or they may be the cause of a relapse of the disease at a later date. Interference with growth is comparatively common, and may involve only the epiphysial junctions in the immediate vicinity of the joint affected, or those of all the bones of the limb. This is well seen in adults who have suffered from severe disease of the hip in childhood—the entire limb, including the foot, being shorter and smaller than the corresponding parts of the opposite side.
Atrophic conditions are also met with, the bones undergoing fatty atrophy, so that in extreme cases they may be cut with a knife or be easily fractured. These atrophic conditions are most marked in bedridden patients, and are largely due to disuse of the limb; they are recovered from if it is able to resume its functions.
Clinical Features.—These vary with the different anatomical forms of the disease, and with the joint affected.
Sometimes the disease is ushered in by a febrile attack attended with pains in several joints—described by John Duncan as tuberculous arthritic fever. This is liable to be mistaken for rheumatic fever, from which, however, it differs in that there is no real migration from joint to joint; there is an absence of sweating and of cardiac complications; and no benefit follows the administration of salicylates.
In exceptional cases, tuberculous joint disease follows an acute course resembling that of the pyogenic arthritis of infants. This has been observed in children, especially in the knee, the lesion being in the synovial membrane, and attended with an accumulation of pus in the joint. If promptly treated by incision and drainage, recovery is rapid, and free movement of the joint, may be preserved.
The onset and early stages of tuberculous disease, however, are more often insidious, and are attended with so few symptoms that the disease may have obtained a considerable hold before it attracts notice. It is not uncommon for patients or their friends to attribute the condition to injury, as it often first attracts attention after some slight trauma or excessive use of the limb. The symptoms usually subside under rest, only to relapse again with use of the limb.
The initial local symptoms may be due to the presence of a focus in the neighbouring bone, perhaps causing neuralgic pains in the joint, or weakness, tiredness, stiffness, and inability to use the limb, these symptoms improving with rest and being aggravated by exertion.
It is rarely possible by external examination to recognise deep-seated osseous foci in the vicinity of joints; but if they are near the surface in a superficial bone—such as the head of the tibia—there may be local thickening of the periosteum, œdema, pain, and tenderness on pressure and on percussion.
X-ray Appearances of Tuberculous Joints.—Gross lesions such as caseous foci in the marrow of the adjacent bone show as clear areas with an ill-defined margin; a sclerosed focus gives a denser shadow than the surrounding bone, and a sequestrum presents a dark shadow of irregular contour, and a clear interval between it and the surrounding bone.
Caries of the articular surface imparts a woolly appearance or irregular contour in place of the well-defined outline of the articular end of the bone. In bony ankylosis the shadow of the two bones is a continuous one, the joint interval having been filled up. The minor changes are best appreciated on comparison with the normal joint of the other limb.
Wasting of muscles is a constant accompaniment of tuberculous joint disease. It is to be attributed partly to want of use, but chiefly to reflex interference with the trophic innervation of the muscles. It is specially well seen in the extensor and adductor muscles of the thigh in disease of the knee, and in the deltoid in disease of the shoulder. The muscles become soft and flaccid, they exhibit tremors on attempted movement, and their excitability to the faradic current is diminished. The muscular tissue may be largely replaced by fat.
Impairment of the normal movements is one of the most valuable diagnostic signs, particularly in deeply seated joints such as the shoulder, hip, and spine. It is due to a protective contraction of the muscles around the joint, designed to prevent movement. This muscular fixation disappears under anæsthesia.
Abnormal attitudes of the limb occur earlier, and are more pronounced in cases in which pain and other irritative symptoms of articular disease are well marked, and are best illustrated by the attitudes assumed in disease of the hip. They are due to reflex or involuntary contraction of the muscles acting on the joint, with the object of placing it in the attitude of greatest ease; they also disappear under anæsthesia. With the lapse of time they not only become exaggerated, but may become permanent from ankylosis or from contracture of the soft parts round the joint.
Startings at night are to be regarded as an indication that there is progressive disease involving the articular surfaces.
The formation of extra-articular abscess may take place early, or it may not occur till long after the disease has subsided. The abscess may develop so insidiously that it does not attract attention until it has attained considerable size, especially when associated with disease of the spine, pelvis, or hip. The position of the abscess in relation to different joints is fairly constant and is determined by the anatomical relationships of the capsule and synovial membrane to the surrounding tissues. The bursæ and tendon sheaths in the vicinity may influence the direction of spread of the abscess and the situation of resulting sinuses. When the abscess is allowed to burst, or is opened and becomes infected with pyogenic bacteria, there is not only the risk of aggravation of the disease and persistent suppuration, but there is a greater liability to general tuberculosis.
The sinuses may be so tortuous that a probe cannot be passed to the primary focus of disease, and their course and disposition can only be demonstrated by injecting the sinuses with an emulsion of bismuth and taking X-ray photographs.
Tuberculous infection of the lymph glands of the limb is exceptional, but may follow upon infection of the skin around the orifice of a sinus.
A slight rise of temperature in the evening may be induced in quiescent joint lesions by injury or by movement of the joint under anæsthesia, or by the fatigue of a railway journey. When sinuses have formed and become infected with pyogenic bacteria, there may be a diurnal variation in the temperature of the type known as hectic fever (Fig. 11).
Relative Frequency of Tuberculous Disease in Different Joints.—Hospital statistics show that joints are affected in the following order of frequency: Spine, knee, hip, ankle and tarsus, elbow, wrist, shoulder. The hip and spine are most often affected in childhood and youth, the shoulder and wrist in adults; the knee, ankle, and elbow show little age preference.
Clinical Variations of Tuberculous Joint Disease.—The above description applies to tuberculous joint disease in general; it must be modified to include special manifestations or varieties.
When the main incidence of the infection affects the synovial membrane, the clinical picture may assume the form of a hydrops, or of an empyema in which the joint is filled with pus. More common than either of these is the well-known white swelling or tumor albus (Wiseman, 1676) which is the clinical manifestation of diffuse thickening of the synovial membrane along with mucoid degeneration of the peri-synovial cellular tissue. It is well seen in joints which are superficial—such as the knee, ankle, elbow, and wrist. The swelling, which is the first and most prominent clinical feature, develops gradually and painlessly, obliterating the bony prominences by filling up the natural hollows. It appears greater to the eye than is borne out by measurement, being thrown into relief by the wasting of the muscles above and below the joint. In the early stage the swelling is elastic, doughy, and non-sensitive, and corresponds to the superficial area of the synovial membrane involved, and there is comparatively little complaint on the part of the patient, because the articular surfaces and ligaments are still intact. There may be a feeling of weight in the limb, and in the case of the knee and ankle the patient tires on walking and drags the leg with more or less of a limp. Movements of the joint are permitted, but are limited in range. The disability is increased by use and exertion, but, for a time at least, it improves under rest.
If the disease is not arrested, there follow the symptoms and signs of involvement of the articular surfaces.
Influence of Tuberculous Joint Disease on the General Health.—Experience shows that the early stages of tuberculous joint disease are compatible with the appearance of good health. As a rule, however, and especially if there is mixed infection, the health suffers, the appetite is impaired, the patient is easily tired, and there may be some loss of weight.
Treatment.—In addition to the general treatment of tuberculosis, local measures are employed. These may be described under two heads—the conservative and the operative.
Conservative treatment is almost always to be employed in the first instance, as by it a larger proportion of cures is obtained with a smaller mortality and with better functional results than by operation.
Treatment by rest implies the immobilisation of the diseased limb until pain and tenderness have disappeared. The attitude in which the limb is immobilised should be that in which, in the event of subsequent stiffness, it will be most serviceable to the patient. Immobilisation may be secured by bandages, splints, extension, or other apparatus. Extension with weight and pulley is of value in securing rest, especially in disease of the hip or knee; it eliminates muscular spasm, relieves pain and startings at night, and prevents abnormal attitudes of the limb. If, when the patient first comes under observation, the limb is in a deformed attitude which does not readily yield to extension, the deformity should be corrected under an anæsthetic.
The induction of hyperæmia is often helpful, the rubber bandage or the hot-air chamber being employed for an hour or so morning and evening.
Injection of Iodoform.—This is carried out on the same lines as have been described for tuberculous abscess. After the fluid contents of the joint are withdrawn, the iodoform is injected; and this may require to be repeated in a month or six weeks.
After the injection of iodoform there is usually considerable reaction, attended with fever (101° F.), headache, and malaise, and considerable pain and swelling of the joint. In some cases there is sickness, and there may be blood pigment in the urine. The severity of these phenomena diminishes with each subsequent injection.
The use of Scott's dressing and of blisters and of the actual cautery has largely gone out of fashion, but the cautery may still be employed with benefit for the relief of pain in cases in which ulceration of cartilage is a prominent feature.
The application of the X-rays has proved beneficial in synovial lesions in superficial joints such as the wrist or elbow; prolonged exposures are made at fortnightly intervals, and on account of the cicatricial contraction which attends upon recovery, the joint must be kept in good position.
Conservative treatment is only abandoned if improvement does not show itself after a thorough trial, or if the disease relapses after apparent cure.
Operative Treatment.—Other things being equal, operation is more often indicated in adults than in children, because after the age of twenty there is less prospect of recovery under conservative treatment, there is more tendency for the disease to relapse and to invade the internal organs, and there is no fear of interfering with the growth of the bones. The state of the general health may necessitate operation as the most rapid method of removing the disease. The social status of the patient must also be taken into account; the bread-winner, under existing social conditions, may be unable to give up his work for a sufficient time to give conservative measures a fair trial.
The local conditions which decide for or against operation are differently regarded by different surgeons, but it may be said in general terms that operative interference is indicated in cases in which the disease continues to progress in spite of a fair trial of conservative measures; in cases unsuited for conservative treatment—that is to say, where there are severe bone lesions. Operative interference is indicated also when the functional result will be better than that likely to be obtained by conservative measures, as is often the case in the knee and elbow. Cold abscesses should, if possible, be dealt with before operating on the joint.
In many cases the extent of the operation can only be decided after exploration. The aim is to remove all the disease with the least impairment of function and the minimum sacrifice of healthy tissue. The more open the method of operating the better, so that all parts of the joint may be available for inspection. The methods of Kocher, which permit of dislocating the joint, are specially to be recommended, as this procedure affords the freest possible access. Diseased synovial membrane is removed with the scissors or knife. If the cartilages are sound, and if a movable joint is aimed at, they may be left; but if ankylosis is desired, they must be removed. Localised disease of the cartilage should be removed with the spoon or gouge, and the bone beneath investigated. If the articular surface is extensively diseased, a thin slice of bone should be removed, and if foci in the marrow are then revealed, it is better to gouge them out than to remove further slices of bone, as this involves sacrifice of the cortex and periosteum.
Operative treatment of deformities resulting from tuberculous joint disease has almost entirely replaced reduction by force; the contracted soft parts are divided, and the bone is resected.
Amputation for tuberculous joint disease has become one of the rare operations of surgery, and is only justified when less radical measures have failed and the condition of the limb is affecting the general health. Amputation is more frequently called for in persons past middle life who are the subjects of pulmonary tuberculosis.