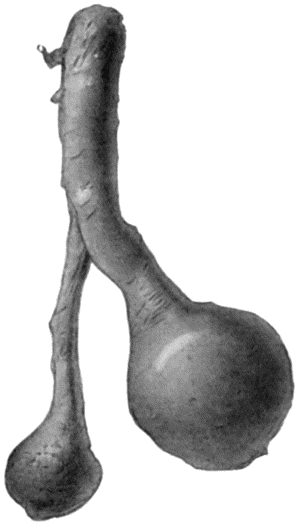
Fig. 84.—Stump Neuromas of Sciatic Nerve, excised forty years after the original amputation by Mr. A. G. Miller.
Nerves are liable to be cut or torn across, bruised, compressed, stretched, or torn away from their connections with the spinal medulla.
Complete Division of a Mixed Nerve.—Complete division is a common result of accidental wounds, especially above the wrist, where the ulnar, median, and radial nerves are frequently cut across, and in gun-shot injuries.
Changes in Structure and Function.—The mere interruption of the continuity of a nerve results in degeneration of its fibres, the myelin being broken up into droplets and absorbed, while the axis cylinders swell up, disintegrate, and finally disappear. Both the conducting and the insulating elements are thus lost. The degeneration in the central end of the divided nerve is usually limited to the immediate proximity of the lesion, and does not even involve all the nerve fibres. In the distal end, it extends throughout the entire peripheral distribution of the nerve, and appears to be due to the cutting off of the fibres from their trophic nerve cells in the spinal medulla. Immediate suturing of the ends does not affect the degeneration of the distal segment. The peripheral end undergoes complete degeneration in from six weeks to two months.
The physiological effects of complete division are that the muscles supplied by the nerve are immediately paralysed, the area to which it furnishes the sole cutaneous supply becomes insensitive, and the other structures, including tendons, bones, and joints, lose sensation, and begin to atrophy from loss of the trophic influence.
Nerves divided in Amputation.—In the case of nerves divided in an amputation, there is an active, although necessarily abortive, attempt at regeneration, which results in the formation of bulbous swellings at the cut ends of the nerves. When there has been suppuration, and especially if the nerves have been cut so as to be exposed in the wound, these bulbous swellings may attain an abnormal size, and are then known as “amputation” or “stump neuromas” (Fig. 84).
When the nerves in a stump have not been cut sufficiently short, they may become involved in the cicatrix, and it may be necessary, on account of pain, to free them from their adhesions, and to resect enough of the terminal portions to prevent them again becoming adherent. When this is difficult, a portion may be resected from each of the nerve-trunks at a higher level; and if this fails to give relief, a fresh amputation may be performed. When there is agonising pain dependent upon an ascending neuritis, it may be necessary to resect the corresponding posterior nerve roots within the vertebral canal.

Fig. 84.—Stump Neuromas of Sciatic Nerve, excised forty years after the original amputation by Mr. A. G. Miller.
Other Injuries of Nerves.—Contusion of a nerve-trunk is attended with extravasation of blood into the connective-tissue sheaths, and is followed by degeneration of the contused nerve fibres. Function is usually restored, the conducting paths being re-established by the formation of new nerve fibres.
When a nerve is torn across or badly crushed—as, for example, by a fractured bone—the changes are similar to those in a divided nerve, and the ultimate result depends on the amount of separation between the ends and the possibility of the young axis cylinders bridging the gap.
Involvement of Nerves in Scar Tissue.—Pressure or traction may be exerted upon a nerve by contracting scar tissue, or a process of neuritis or perineuritis may be induced.
When terminal filaments are involved in a scar, it is best to dissect out the scar, and along with it the ends of the nerves pressed upon. When a nerve-trunk, such as the sciatic, is involved in cicatricial tissue, the nerve must be exposed and freed from its surroundings (neurolysis), and then stretched so as to tear any adhesions that may be present above or below the part exposed. It may be advisable to displace the liberated nerve from its original position so as to minimise the risk of its incorporation in the scar of the original wound or in that resulting from the operation—for example, the radial nerve may be buried in the substance of the triceps, or it may be surrounded by a segment of vein or portion of fat-bearing fascia.
Injuries of nerves resulting from gun-shot wounds include: (1) those in which the nerve is directly damaged by the bullet, and (2) those in which the nerve-trunk is involved secondarily either by scar tissue in its vicinity or by callus following fracture of an adjacent bone. The primary injuries include contusion, partial or complete division, and perforation of the nerve-trunk. One of the most constant symptoms is the early occurrence of severe neuralgic pain, and this is usually associated with marked hyperæsthesia.
Regeneration.—Process of Repair when the Ends are in Contact.—If the wound is aseptic, and the ends of the divided nerve are sutured or remain in contact, they become united, and the conducting paths are re-established by a regeneration of nerve fibres. There is a difference of opinion as to the method of regeneration. The Wallerian doctrine is that the axis cylinders in the central end grow downwards, and enter the nerve sheaths of the distal portion, and continue growing until they reach the peripheral terminations in muscle and skin, and in course of time acquire a myelin sheath; the cells of the neurolemma multiply and form long chains in both ends of the nerve, and are believed to provide for the nourishment and support of the actively lengthening axis cylinders. Another view is that the formation of new axis cylinders is not confined to the central end, but that it goes on also in the peripheral segment, in which, however, the new axis cylinders do not attain maturity until continuity with the central end has been re-established.
If the wound becomes infected and suppuration occurs, the young nerve fibres are destroyed and efficient regeneration is prevented; the formation of scar tissue also may constitute a permanent obstacle to new nerve fibres bridging the gap.
When the ends are not in contact, reunion of the divided nerve fibres does not take place whether the wound is infected or not. At the proximal end there forms a bulbous swelling, which becomes adherent to the scar tissue. It consists of branching axis cylinders running in all directions, these having failed to reach the distal end because of the extent of the gap. The peripheral end is completely degenerated, and is represented by a fibrous cord, the cut end of which is often slightly swollen or bulbous, and is also incorporated with the scar tissue of the wound.
Clinical Features.—The symptoms resulting from division and non-union of a nerve-trunk necessarily vary with the functions of the affected nerve. The following description refers to a mixed sensori-motor trunk, such as the median or radial (musculo-spiral) nerve.
Sensory Phenomena.—Superficial touch is tested by means of a wisp of cotton wool stroked gently across the skin; the capacity of discriminating two points as separate, by a pair of blunt-pointed compasses; the sensation of pressure, by means of a pencil or other blunt object; of pain, by pricking or scratching with a needle; and of sensibility to heat and cold, by test-tubes containing water at different temperatures. While these tests are being carried out, the patient's eyes are screened off.
After division of a nerve containing sensory fibres, there is an area of absolute cutaneous insensibility to touch (anæsthesia), to pain (analgesia), and to all degrees of temperature—loss of protopathic sensibility; surrounded by an area in which there is loss of sensation to light touch, inability to recognise minor differences of temperature (72°–104° F.), and to appreciate as separate impressions the contact of the two points of a compass—loss of epicritic sensibility (Head and Sherren) (Figs. 91, 92).
Motor Phenomena.—There is immediate and complete loss of voluntary power in the muscles supplied by the divided nerve. The muscles rapidly waste, and within from three to five days, they cease to react to the faradic current. When tested with the galvanic current, it is found that a stronger current must be used to call forth contraction than in a healthy muscle, and the contraction appears first at the closing of the circuit when the anode is used as the testing electrode. The loss of excitability to the interrupted current, and the specific alteration in the type of contraction with the constant current, is known as the reaction of degeneration. After a few weeks all electric excitability is lost. The paralysed muscles undergo fatty degeneration, which attains its maximum three or four months after the division of the nerve. Further changes may take place, and result in the transformation of the muscle into fibrous tissue, which by undergoing shortening may cause deformity known as paralytic contracture.
Vaso-motor Phenomena.—In the majority of cases there is an initial rise in the temperature of the part (2° to 3° F.), with redness and increased vascularity. This is followed by a fall in the local temperature, which may amount to 8° or 10° F., the parts becoming pale and cold. Sometimes the hyperæmia resulting from vaso-motor paralysis is more persistent, and is associated with swelling of the parts from œdema—the so-called angio-neurotic œdema. The vascularity varies with external influences, and in cold weather the parts present a bluish appearance.
Trophic Phenomena.—Owing to the disappearance of the subcutaneous fat, the skin is smooth and thin, and may be abnormally dry. The hair is harsh, dry, and easily shed. The nails become brittle and furrowed, or thick and curved, and the ends of the fingers become club-shaped. Skin eruptions, especially in the form of blisters, occur, or there may be actual ulcers of the skin, especially in winter. In aggravated cases the tips of the fingers disappear from progressive ulceration, and in the sole of the foot a perforating ulcer may develop. Arthropathies are occasionally met with, the joints becoming the seat of a painless effusion or hydrops, which is followed by fibrous thickening of the capsular and other ligaments, and terminates in stiffness and fibrous ankylosis. In this way the fingers are seriously crippled and deformed.
Treatment of Divided Nerves.—The treatment consists in approximating the divided ends of the nerve and placing them under the most favourable conditions for repair, and this should be done at the earliest possible opportunity. (Op. Surg., pp. 45, 46.)
Primary Suture.—The reunion of a recently divided nerve is spoken of as primary suture, and for its success asepsis is essential. As the suturing of the ends of the nerve is extremely painful, an anæsthetic is required.
When the wound is healed and while waiting for the restoration of function, measures are employed to maintain the nutrition of the damaged nerve and of the parts supplied by it. The limb is exercised, massaged, and douched, and protected from cold and other injurious influences. The nutrition of the paralysed muscles is further improved by electricity. The galvanic current is employed, using at first a mild current of not more than 5 milliampères for about ten minutes, the current being made to flow downwards in the course of the nerve, with the positive electrode applied to the spine, and the negative over the affected nerve near its termination. It is an advantage to have a metronome in the circuit whereby the current is opened and closed automatically at intervals, so as to cause contraction of the muscles.
The results of primary suture, when it has been performed under favourable conditions, are usually satisfactory. In a series of cases investigated by Head and Sherren, the period between the operation and the first return of sensation averaged 65 days. According to Purves Stewart protopathic sensation commences to appear in about six weeks and is completely restored in six months; electric sensation and motor power reappear together in about six months, and restoration is complete in a year. When sensation returns, the area of insensibility to pain steadily diminishes and disappears; sensibility to extremes of temperature appears soon after; and last of all, after a considerable interval, there is simultaneous return of appreciation of light touch, moderate degrees of temperature, and the points of a compass.
A clinical means of estimating how regeneration in a divided nerve is progressing has been described by Tinel. He found that a tingling sensation, similar to that experienced in the foot, when it is recovering from the “sleeping” condition induced by prolonged pressure on the sciatic nerve from sitting on a hard bench, can be elicited on percussing over growing axis cylinders. Tapping over the proximal end of a newly divided nerve, e.g. the common peroneal behind the head of the fibula, produces no tingling, but when in about three weeks axis cylinders begin to grow in the proximal end-bulb, local tingling is induced by tapping there. The downward growth of the axis cylinders can be traced by tapping over the distal segment of the nerve, the tingling sensation being elicited as far down as the young axis cylinders have reached. When the regeneration of the axis cylinders is complete, tapping no longer causes tingling. It usually takes about one hundred days for this stage to be reached.
Tinel's sign is present before voluntary movement, muscular tone, or the normal electrical reactions reappear.
In cases of complete nerve paralysis that have not been operated upon, the tingling test is helpful in determining whether or not regeneration is taking place. Its detection may prevent an unnecessary operation being performed.
Primary suture should not be attempted so long as the wound shows signs of infection, as it is almost certain to end in failure. The ends should be sutured, however, as soon as the wound is aseptic or has healed.
Secondary Suture.—The term secondary suture is applied to the operation of stitching the ends of the divided nerve after the wound has healed.
Results of Secondary Suture.—When secondary suture has been performed under favourable conditions, the prognosis is good, but a longer time is required for restoration of function than after primary suture. Purves Stewart says protopathic sensation is sometimes observed much earlier than in primary suture, because partial regeneration of axis cylinders in the peripheral segment has already taken place. Sensation is recovered first, but it seldom returns before three or four months. There then follows an improvement or disappearance of any trophic disturbances that may be present. Recovery of motion may be deferred for long periods—rather because of the changes in the muscles than from want of conductivity in the nerve—and if the muscles have undergone complete degeneration, it may never take place at all. While waiting for recovery, every effort should be made to maintain the nutrition of the damaged nerve, and of the parts which it supplies.
When suture is found to be impossible, recourse must be had to other methods, known as nerve bridging and nerve implantation.
Incomplete Division of a Mixed Nerve.—The effects of partial division of a mixed nerve vary according to the destination of the nerve bundles that have been interrupted. Within their area of distribution the paralysis is as complete as if the whole trunk had been cut across. The uninjured nerve-bundles continue to transmit impulses with the result that there is a dissociated paralysis within the distribution of the affected nerve, some muscles continuing to act and to respond normally to electric stimulation, while others behave as if the whole nerve-trunk had been severed.
In addition to vasomotor and trophic changes, there is often severe pain of a burning kind (causalgia or thermalgia) which comes on about a fortnight after the injury and causes intense and continuous suffering which may last for months. Paroxysms of pain may be excited by the slightest touch or by heat, and the patient usually learns for himself that the constant application of cold wet cloths allays the pain. The thermalgic area sweats profusely.
Operative treatment is indicated where there is no sign of improvement within three months, when recovery is arrested before complete restoration of function is attained, or when thermalgic pain is excessive.
Subcutaneous Injuries of Nerves.—Several varieties of subcutaneous injuries of nerves are met with. One of the best known is the compression paralysis of the nerves of the upper arm which results from sleeping with the arm resting on the back of a chair or the edge of a table—the so-called “drunkard's palsy”; and from the pressure of a crutch in the axilla—“crutch paralysis.” In some of these injuries, notably “drunkard's palsy,” the disability appears to be due not to damage of the nerve, but to overstretching of the extensors of the wrist and fingers (Jones). A similar form of paralysis is sometimes met with from the pressure of a tourniquet, from tight bandages or splints, from the pressure exerted by a dislocated bone or by excessive callus, and from hyper-extension of the arm during anæsthesia.
In all these forms there is impaired sensation, rarely amounting to anæsthesia, marked muscular wasting, and diminution or loss of voluntary motor power, while—and this is a point of great importance—the normal electrical reactions are preserved. There may also develop trophic changes such as blisters, superficial ulcers, and clubbing of the tips of the fingers. The prognosis is usually favourable, as recovery is the rule within from one to three months. If, however, neuritis supervenes, the electrical reactions are altered, the muscles degenerate, and recovery may be retarded or may fail to take place.
Injuries which act abruptly or instantaneously are illustrated in the crushing of a nerve by the sudden displacement of a sharp-edged fragment of bone, as may occur in comminuted fractures of the humerus. The symptoms include perversion or loss of sensation, motor paralysis, and atrophy of muscles, which show the reaction of degeneration from the eighth day onwards. The presence of the reaction of degeneration influences both the prognosis and the treatment, for it implies a lesion which is probably incapable of spontaneous recovery, and which can only be remedied by operation.
The treatment varies with the cause and nature of the lesion. When, for example, a displaced bone or a mass of callus is pressing upon the nerve, steps must be taken to relieve the pressure, by operation if necessary. When there is reason to believe that the nerve is severely crushed or torn across, it should be exposed by incision, and, after removal of the damaged ends, should be united by sutures. When it is impossible to make a definite diagnosis as to the state of the nerve, it is better to expose it by operation, and thus learn the exact state of affairs without delay; in the event of the nerve being torn, the ends should be united by sutures.
Dislocation of Nerves.—This injury, which resembles the dislocation of tendons from their grooves, is seldom met with except in the ulnar nerve at the elbow, and is described with injuries of that nerve.