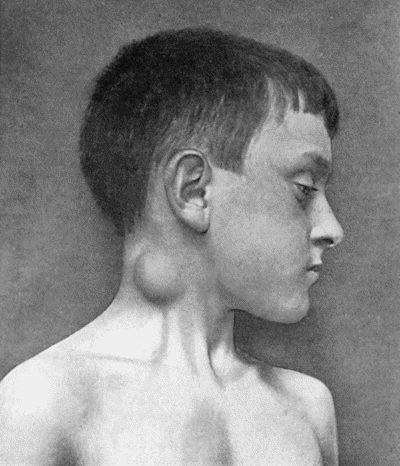
Fig. 77.—Tuberculous Cervical Gland with abscess formation in subcutaneous cellular tissue, in a boy æt. 10.
Lymphadenitis.—Inflammation of lymph glands results from the advent of an irritant, usually bacterial or toxic, brought to the glands by the afferent lymph vessels. These vessels may share in the inflammation and be the seat of lymphangitis, or they may show no evidence of the passage of the noxa. It is exceptional for the irritant to reach the gland through the blood-stream.
A strain or other form of trauma is sometimes blamed for the onset of lymphadenitis, especially in the glands of the groin (bubo), but it is usually possible to discover some source of pyogenic infection which is responsible for the mischief, or to obtain a history of some antecedent infection such as gonorrhœa. It is possible for gonococci to lie latent in the inguinal glands for long periods, and only give rise to lymphadenitis if the glands be subsequently subjected to injury. The glands most frequently affected are those in the neck, axilla, and groin.
The characters of the lymphadenitis vary with the nature of the irritant. Sometimes it is mild and evanescent, as in the glandular enlargement in the neck which attends tonsillitis and other forms of sore throat. Sometimes it is more persistent, as in the enlargement that is associated with adenoids, hypertrophied tonsils, carious teeth, eczema of the scalp, and otorrhœa; and it is possible that this indolent enlargement predisposes to tuberculous infection. A similar enlargement is met with in the axilla in cases of chronic interstitial mastitis, and in the groin as a result of chronic irritation about the external genitals, such as balanitis.
Sometimes the lymphadenitis is of an acute character, and the tendency is towards the formation of an abscess. This is illustrated in the axillary glands as a result of infected wounds of the fingers; in the femoral glands in infected wounds or purulent blisters on the foot; in the inguinal glands in gonorrhœa and soft sore; and in the cervical glands in the severer forms of sore throat associated with diphtheria and scarlet fever. The most acute suppurations result from infection with streptococci.
Superficial glands, when inflamed and suppurating, become enlarged, tender, fixed, and matted to one another. In the glands of the groin the suppurative process is often remarkably sluggish; purulent foci form in the interior of individual glands, and some time may elapse before the pus erupts through their respective capsules. In the deeply placed cervical glands, especially in cases of streptococcal throat infections, the suppuration rapidly involves the surrounding cellular tissue, and the clinical features are those of an acute cellulitis and deeply seated abscess. When this is incised the necrosed glands may be found lying in the pus, and on bacteriological examination are found to be swarming with streptococci. In suppuration of the axillary glands the abscess may be quite superficial, or it may be deeply placed beneath the strong fascia and pectoral muscles, according to the group of glands involved.
The diagnosis of septic lymphadenitis is usually easy. The indolent enlargements are not always to be distinguished, however, from commencing tuberculous disease, except by the use of the tuberculin test, and by the fact that they usually disappear on removing the peripheral source of irritation.
Treatment.—The first indication is to discover and deal with the source of infection, and in the indolent forms of lymphadenitis this will usually be followed by recovery. In the acute forms following on pyogenic infection, the best results are obtained from the hyperæmic treatment carried out by means of suction bells. If suppuration is not thereby prevented, or if it has already taken place, each separate collection of pus is punctured with a narrow-bladed knife and the use of the suction bell is persevered with. If there is a large periglandular abscess, as is often the case, in the neck and axilla, the opening may require to be made by Hilton's method, and it may be necessary to insert a drainage-tube.

Fig. 77.—Tuberculous Cervical Gland with abscess formation in subcutaneous cellular tissue, in a boy æt. 10.
Tuberculous Disease of Glands.—This is a disease of great frequency and importance. The tubercle bacilli usually gain access to the gland through the afferent lymph vessels, which convey them from some lesion of the surface within the area drained by them. Tuberculous infection may supervene in glands that are already enlarged as a result of chronic septic irritation. While any of the glands in the body may be affected, the disease is most often met with in the cervical groups which derive their lymph from the mouth, nose, throat, and ear.
The appearance of the glands on section varies with the stage of the disease. In the early stages the gland is enlarged, it may be to many times its natural size, is normal in appearance and consistence, and as there is no peri-adenitis it is easily shelled out from its surroundings. On microscopical examination, however, there is evidence of infection in the shape of bacilli and of characteristic giant and epithelioid cells. At a later stage, the gland tissue is studded with minute yellow foci which tend to enlarge and in time to become confluent, so that the whole gland is ultimately converted into a caseous mass. This caseous material is surrounded by the thickened capsule which, as a result of peri-adenitis, tends to become adherent to and fused with surrounding structures, and particularly with layers of fascia and with the walls of veins. The caseated tissue often remains unchanged for long periods; it may become calcified, but more frequently it breaks down and liquefies.
Tuberculous disease in the cervical glands is a common accompaniment or sequel of adenoids, enlarged tonsils, carious teeth, pharyngitis, middle-ear disease, and conjunctivitis. These lesions afford the bacilli a chance of entry into the lymph vessels, in which they are carried to the glands, where they give rise to disease.
The enlargement may affect only one gland, usually below the angle of the mandible, and remain confined to it, the gland reaching the size of a hazel-nut, and being ovoid, firm, and painless. More commonly the disease affects several glands, on one or on both sides of the neck. When the disease commences in the pre-auricular or submaxillary glands, it tends to spread to those along the carotid sheath: when the posterior auricular and occipital glands are first involved, the spread is to those along the posterior border of the sterno-mastoid. In many cases all the chains in front of, beneath, and behind this muscle are involved, the enlarged glands extending from the mastoid to the clavicle. They are at first discrete and movable, and may even vary in size from time to time; but with the addition of peri-adenitis they become fixed and matted together, forming lobulated or nodular masses (Fig. 78). They become adherent not only to one another, but also to the structures in their vicinity,—and notably to the internal jugular vein,—a point of importance in regard to their removal by operation.
At any stage the disease may be arrested and the glands remain for long periods without further change. It is possible that the tuberculous tissue may undergo cicatrisation. More commonly suppuration ensues, and a cold abscess forms, but if there is a mixed infection, the pyogenic factor being usually derived from the throat, it may take on active features.
The transition from the solid to the liquefied stage is attended with pain and tenderness in the gland, which at the same time becomes fixed and globular, and finally fluctuation can be elicited.
If left to itself, the softened tubercle erupts through the capsule of the gland and infects the cellular tissue. The cervical fascia is perforated and a cold abscess, often much larger than the gland from which it took origin, forms between the fascia and the overlying skin. The further stages—reddening, undermining of skin and external rupture, with the formation of ulcers and sinuses—have been described with tuberculous abscess. The ulcers and sinuses persist indefinitely, or they heal and then break out again; sometimes the skin becomes infected, and a condition like lupus spreads over a considerable area. Spontaneous healing finally takes place after the caseous tubercle has been extruded; the resulting scars are extremely unsightly, being puckered or bridled, or hypertrophied like keloid.
While the disease is most common in childhood and youth, it may be met with even in advanced life; and although often associated with impaired health and unhealthy surroundings, it may affect those who are apparently robust and are in affluent circumstances.
Diagnosis.—The chief importance lies in differentiating tuberculous disease from lympho-sarcoma and from lymphadenoma, and this is usually possible from the history and from the nature of the enlargement. Signs of liquefaction and suppuration support the diagnosis of tubercle. If any doubt remains, one of the glands should be removed and submitted to microscopical examination. Other forms of sarcoma, and the enlargement of an accessory thyreoid, are less likely to be confused with tuberculous glands. Calcified tuberculous glands give definite shadows with the X-rays.
Enlargement of the cervical glands from secondary cancer may simulate tuberculosis, but is differentiated by its association with cancer in the mouth or throat, and by the characteristic, stone-like induration of epithelioma.
The cold abscess which results from tuberculous glands is to be distinguished from that due to disease in the cervical spine, retro-pharyngeal abscess, as well as from congenital and other cystic swellings in the neck.
Prognosis.—Next to lupus, glandular disease is of all tuberculous lesions the least dangerous to life; but while it is the rule to recover from tuberculous disease of glands with or without an operation, it is unfortunately quite common for such persons to become the subjects of tuberculosis in other parts of the body at any subsequent period of life.
Treatment.—There is considerable difference of opinion regarding the treatment of glandular tuberculosis. Some authorities, impressed with the undoubted possibility of natural cure, are satisfied with promoting this by measures directed towards improving the general health, by the prolonged administration of tuberculin, and by repeated exposures to the X-rays and to sunlight. Others again, influenced by the risk of extension of the disease and by the destruction of tissue and disfigurement caused by breaking down of the tuberculous tissue and mixed infection, advocate the removal of the glands by operation.
The conditions vary widely in different cases, and the treatment should be adapted to the individual requirements. If the disease remains confined to the glands originally infected and there are no signs of breaking down, “expectant measures” may be persevered with.
If, on the other hand, the disease exhibits aggressive tendencies, the question of operation should be considered. The undesirable results of the breaking down and liquefaction of the diseased gland may be avoided by the timely withdrawal of the fluid contents through a hollow needle.
The excision of tuberculous glands is often a difficult operation, because of the number and deep situation of the glands to be removed, and of the adhesions to surrounding structures. The skin incision must be sufficiently extensive to give access to the whole of the affected area, and to avoid disfigurement should, whenever possible, be made in the line of the natural creases of the skin. In exposing the glands the common facial and other venous trunks may require to be clamped and tied. Care must be taken not to injure the important nerves, particularly the accessory, the vagus, and the phrenic. The inframaxillary branches of the facial, the hypoglossal and its descending branches, and the motor branches of the deep cervical plexus, are also liable to be injured. The dissection is rendered easier and is attended with less risk of injury to the nerves, if the patient is placed in the sitting posture so as to empty the veins, and, instead of a knife, the conical scissors of Mayo are employed. When the glands are extensively affected on both sides of the neck, it is advisable to allow an interval to elapse rather than to operate on both sides at one sitting. (Op. Surg., p. 189.)
If the tonsils are enlarged they should not be removed at the same time, as, by so doing, there is a risk of pyogenic infection from the throat being carried to the wound in the neck, but they should be removed, after an interval, to prevent relapse of disease in the glands.
When the skin is broken and caseous tuberculous tissue is exposed, healing is promoted by cutting away diseased skin, removing the granulation tissue with the spoon, scraping sinuses, and packing the cavity with iodoform worsted and treating it by the open method and secondary suture if necessary. Exposure to the sunshine on the seashore and to the X-rays is often beneficial in these cases.
Tuberculous disease in the axillary glands may be a result of extension from those in the neck, from the mamma, ribs, or sternum, or more rarely from the upper extremity. We have seen it from an infected wound of a finger. In some cases no source of infection is discoverable. The individual glands attain a considerable size, and they fuse together to form a large tumour which fills up the axillary space. The disease progresses more rapidly than it does in the cervical glands, and almost always goes on to suppuration with the formation of sinuses. Conservative measures need not be considered, as the only satisfactory treatment is excision, and that without delay.
Tuberculous disease in the glands of the groin is comparatively rare. We have chiefly observed it in the femoral glands as a result of inoculation tubercle on the toes or sole of the foot. The affected glands nearly always break down and suppurate, and after destroying the overlying skin give rise to fungating ulcers. The treatment consists in excising the glands and the affected skin. The dissection may be attended with troublesome hæmorrhage from the numerous veins that converge towards the femoral trunk.
Tuberculous disease in the mesenteric and bronchial glands is described with the surgery of regions.
Syphilitic Disease of Glands.—Enlargement of lymph glands is a prominent feature of acquired syphilis, especially in the form of the indolent or bullet-bubo which accompanies the primary lesion, and the general enlargement of glands that occurs in secondary syphilis. Gummatous disease in glands is extremely rare; the affected gland rapidly enlarges to the size of a walnut, and may then persist for a long period without further change; if it breaks down, the overlying skin is destroyed and the caseated tissue of the gumma exposed.
Lymphadenoma.—Hodgkin's Disease (Pseudo-leukæmia of German authors).—This is a rare disease, the origin of which is as yet unknown, but analogy would suggest that it is due to infection with a slowly growing micro-organism. It is chiefly met with in young subjects, and is characterised by a painless enlargement of a particular group of glands, most commonly those in the cervical region (Fig. 80).
The glands are usually larger than in tuberculosis, and they remain longer discrete and movable; they are firm in consistence, and on section present a granular appearance due to overgrowth of the connective-tissue framework. In time the glandular masses may form enormous projecting tumours, the swelling being added to by lymphatic œdema of the overlying cellular tissue and skin.
The enlargement spreads along the chain of glands to those above the clavicle, to those in the axilla, and to those of the opposite side (Fig. 81). Later, the glands in the groin become enlarged, and it is probable that the infection has spread from the neck along the mediastinal, bronchial, retro-peritoneal, and mesenteric glands, and has branched off to the iliac and inguinal groups.
Two clinical types are recognised, one in which the disease progresses slowly and remains confined to the cervical glands for two or more years; the other, in which the disease is more rapidly disseminated and causes death in from twelve to eighteen months.

Fig. 81.—Lymphadenoma (Hodgkin's Disease) affecting left side of neck and left axilla, in a woman æt. 44. Three years' duration.
In the acute form, the health suffers, there is fever, and the glands may vary in size with variations in the temperature; the blood presents the characters met with in secondary anæmia. The spleen, liver, testes, and mammæ may be enlarged; the glandular swellings press on important structures, such as the trachea, œsophagus, or great veins, and symptoms referable to such pressure manifest themselves.
Diagnosis.—Considerable difficulty attends the diagnosis of lymphadenoma at an early stage. The negative results of tuberculin tests may assist in the differentiation from tuberculous disease, but the more certain means of excising one of the suspected glands and submitting it to microscopical examination should be had recourse to. The sections show proliferation of endothelial cells, the formation of numerous giant cells quite unlike those of tuberculosis and a progressive fibrosis. Lympho-sarcoma can usually be differentiated by the rapid assumption of the local features of malignant disease, and in a gland removed for examination, a predominance of small round cells with scanty protoplasm. The enlargement associated with leucocythæmia is differentiated by the characteristic changes in the blood.
Treatment.—In the acute form of lymphadenoma, treatment is of little avail. Arsenic may be given in full doses either by the mouth or by subcutaneous injection; the intravenous administration of neo-salvarsan may be tried. Exposure to the X-rays and to radium has been more successful than any other form of treatment. Excision of glands, although sometimes beneficial, seldom arrests the progress of the disease. The ease and rapidity with which large masses of glands may be shelled out is in remarkable contrast to what is observed in tuberculous disease. Surgical interference may give relief when important structures are being pressed upon—tracheotomy, for example, may be required where life is threatened by asphyxia.
Leucocythæmia.—This is a disease of the blood and of the blood-forming organs, in which there is a great increase in the number, and an alteration of the character, of the leucocytes present in the blood. It may simulate lymphadenoma, because, in certain forms of the disease, the lymph glands, especially those in the neck, axilla, and groin, are greatly enlarged.