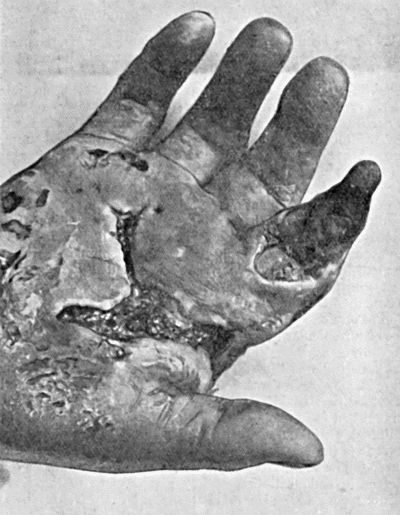
Fig. 22.—Gangrene of Terminal Phalanx of Index-Finger, following cellulitis of hand resulting from a scratch on the palm of the hand.
The acute bacillary forms of gangrene all assume the moist type from the first, and, spreading rapidly, result in extensive necrosis of tissue, and often end fatally.
The infection is usually a mixed one in which anaërobic bacteria predominate. The anaërobe most constantly present is the bacillus ærogenes capsulatus, usually in association with other anaërobes, and sometimes with pyogenic diplo- and streptococci. According to the mode of action of the associated organisms and the combined effects of their toxins on the tissues, the gangrenous process presents different pathological and clinical features. Some combinations, for example, result in a rapidly spreading cellulitis with early necrosis of connective tissue accompanied by thrombosis throughout the capillary and venous circulation of the parts implicated; other combinations cause great œdema of the part, and others again lead to the formation of gases in the tissues, particularly in the muscles.
These different effects do not appear to be due to a specific action of any one of the organisms present, but to the combined effect of a particular group living in symbiosis.
According as the cellulitic, the œdematous, or the gaseous characteristics predominate, the clinical varieties of bacillary gangrene may be separately described, but it must be clearly understood that they frequently overlap and cannot always be distinguished from one another.
Clinical Varieties of Bacillary Gangrene.—Acute infective gangrene is the form most commonly met with in civil practice. It may follow such trivial injuries as a pin-prick or a scratch, the signs of acute cellulitis rapidly giving place to those of a spreading gangrene. Or it may ensue on a severe railway, machinery, or street accident, when lacerated and bruised tissues are contaminated with gross dirt. Often within a few hours of the injury the whole part rapidly becomes painful, swollen, œdematous, and tense. The skin is at first glazed, and perhaps paler than normal, but soon assumes a dull red or purplish hue, and bullæ form on the surface. Putrefactive gases may be evolved in the tissues, and their presence is indicated by emphysematous crackling when the part is handled. The spread of the disease is so rapid that its progress is quite visible from hour to hour, and may be traced by the occurrence of red lines along the course of the lymphatics of the limb. In the most acute cases the death of the affected part takes place so rapidly that the local changes indicative of gangrene have not time to occur, and the fact that the part is dead may be overlooked.

Fig. 22.—Gangrene of Terminal Phalanx of Index-Finger, following cellulitis of hand resulting from a scratch on the palm of the hand.
Rigors may occur, but the temperature is not necessarily raised—indeed, it is sometimes subnormal. The pulse is small, feeble, rapid, and irregular. Unless amputation is promptly performed, death usually follows within thirty-six or forty-eight hours. Even early operation does not always avert the fatal issue, because the quantity of toxin absorbed and its extreme virulence are often more than even a robust subject can outlive.
Treatment.—Every effort must be made to purify all such wounds as are contaminated by earth, street dust, stable refuse, or other forms of gross dirt. Devitalised and contaminated tissue is removed with the knife or scissors and the wound purified with antiseptics of the chlorine group or with hydrogen peroxide. If there is a reasonable prospect that infection has been overcome, the wound may be at once sutured, but if this is doubtful it is left open and packed or irrigated.
When acute gangrene has set in no treatment short of amputation is of any avail, and the sooner this is done, the greater is the hope of saving the patient. The limb must be amputated well beyond the apparent limits of the infected area, and stringent precautions must be taken to avoid discharge from the already gangrenous area reaching the operation wound. An assistant or nurse, who is to take no other part in the operation, is told off to carry out the preliminary purification, and to hold the limb during the operation.
Malignant Œdema.—This form of acute gangrene has been defined as “a spreading inflammatory œdema attended with emphysema, and ultimately followed by gangrene of the skin and adjacent parts.” The predominant organism is the bacillus of malignant œdema or vibrion septique of Pasteur, which is found in garden soil, dung, and various putrefying substances. It is anaërobic, and occurs as long, thick rods with somewhat rounded ends and several laterally placed flagella. Spores, which have a high power of resistance, form in the centre of the rods, and bulge out the sides so as to give the organisms a spindle-shaped outline. Other pathogenic organisms are also present and aid the specific bacillus in its action.
At the bedside it is difficult, if not impossible, to distinguish it from acute infective gangrene. Both follow on the same kinds of injury and run an exceedingly rapid course. In malignant œdema, however, the incidence of the disease is mainly on the superficial parts, which become œdematous and emphysematous, and acquire a marbled appearance with the veins clearly outlined. Early disappearance of sensation is a particularly grave symptom. Bullæ form on the skin, and the tissues have “a peculiar heavy but not putrid odour.” The constitutional effects are extremely severe, and death may ensue within a few hours.
Acute Emphysematous or Gas Gangrene was prevalent in certain areas at various periods during the European War. It follows infection of lacerated wounds with the bacillus ærogenes capsulatus, usually in combination with other anaërobes, and its main incidence is on the muscles, which rapidly become infiltrated with gas that spreads throughout the whole extent of the muscle, disintegrating its fibres and leading to necrosis. The gangrenous process spreads with appalling rapidity, the limb becoming enormously swollen, painful, and crepitant or even tympanitic. Patches of coppery or purple colour appear on the skin, and bullæ containing blood-stained serum form on the surface. The toxæmia is profound, and the face and lips assume a characteristic cyanosis. The condition is attended with a high mortality. Only in the early stages and when the infection is limited are local measures successful in arresting the spread; in more severe cases amputation is the only means of saving life.
Cancrum Oris or Noma.—This disease is believed to be due to a specific bacillus, which occurs in long delicate rods, and is chiefly found at the margin of the gangrenous area. It is prone to attack unhealthy children from two to five years of age, especially during their convalescence from such diseases as measles, scarlet fever, or typhoid, but may attack adults when they are debilitated. It is most common in the mouth, but sometimes occurs on the vulva. In the mouth it begins as an ulcerative stomatitis, more especially affecting the gums or inner aspect of the cheek. The child lies prostrated, and from the open mouth foul-smelling saliva, streaked with blood, escapes; the face is of an ashy-grey colour, the lips dark and swollen. On the inner aspect of the cheek is a deeply ulcerated surface, with sloughy shreds of dark-brown or black tissue covering its base; the edges are irregular, firm, and swollen, and the surrounding mucous membrane is infiltrated and œdematous. In the course of a few hours a dark spot appears on the outer aspect of the cheek, and rapidly increases in size; towards the centre it is black, shading off through blue and grey into a dark-red area which extends over the cheek (Fig. 23). The tissue implicated is at first firm and indurated, but as it loses its vitality it becomes doughy and sodden. Finally a slough forms, and, when it separates, the cheek is perforated.
Meanwhile the process spreads inside the mouth, and the gums, the floor of the mouth, or even the jaws, may become gangrenous and the teeth fall out. The constitutional disturbance is severe, the temperature raised, and the pulse feeble and rapid.
The extremely fœtid odour which pervades the room or even the house the patient occupies, is usually sufficient to suggest the diagnosis of cancrum oris. The odour must not be mistaken for that due to decomposition of sordes on the teeth and gums of a debilitated patient.
The prognosis is always grave in the extreme, the main risks being general toxæmia and septic pneumonia. When recovery takes place there is serious deformity, and considerable portions of the jaws may be lost by necrosis.
Treatment.—The only satisfactory treatment is thorough removal under an anæsthetic of all the sloughy tissue, with the surrounding zone in which the organisms are active. This is most efficiently accomplished by the knife or scissors, cutting until the tissue bleeds freely, after which the raw surface is painted with undiluted carbolic acid and dressed with iodoform gauze. It may be necessary to remove large pieces of bone when the necrotic process has implicated the jaws. The mouth must be constantly sprayed with peroxide of hydrogen, and washed out with a disinfectant and deodorant lotion, such as Condy's fluid. The patient's general condition calls for free stimulation.
The deformity resulting from these necessarily heroic measures is not so great as might be expected, and can be further diminished by plastic operations, which should be undertaken before cicatricial contraction has occurred.